Across Africa and Asia, an estimated one million women are living with devastating childbirth injuries that cause incontinence—waiting for the care they so desperately need.
To reach these women, we’ve designed our approach with both urgency and sustainability in mind:
First, we fund high-quality surgeries through trusted local partners across 35+ countries—delivering life-changing care to women today.
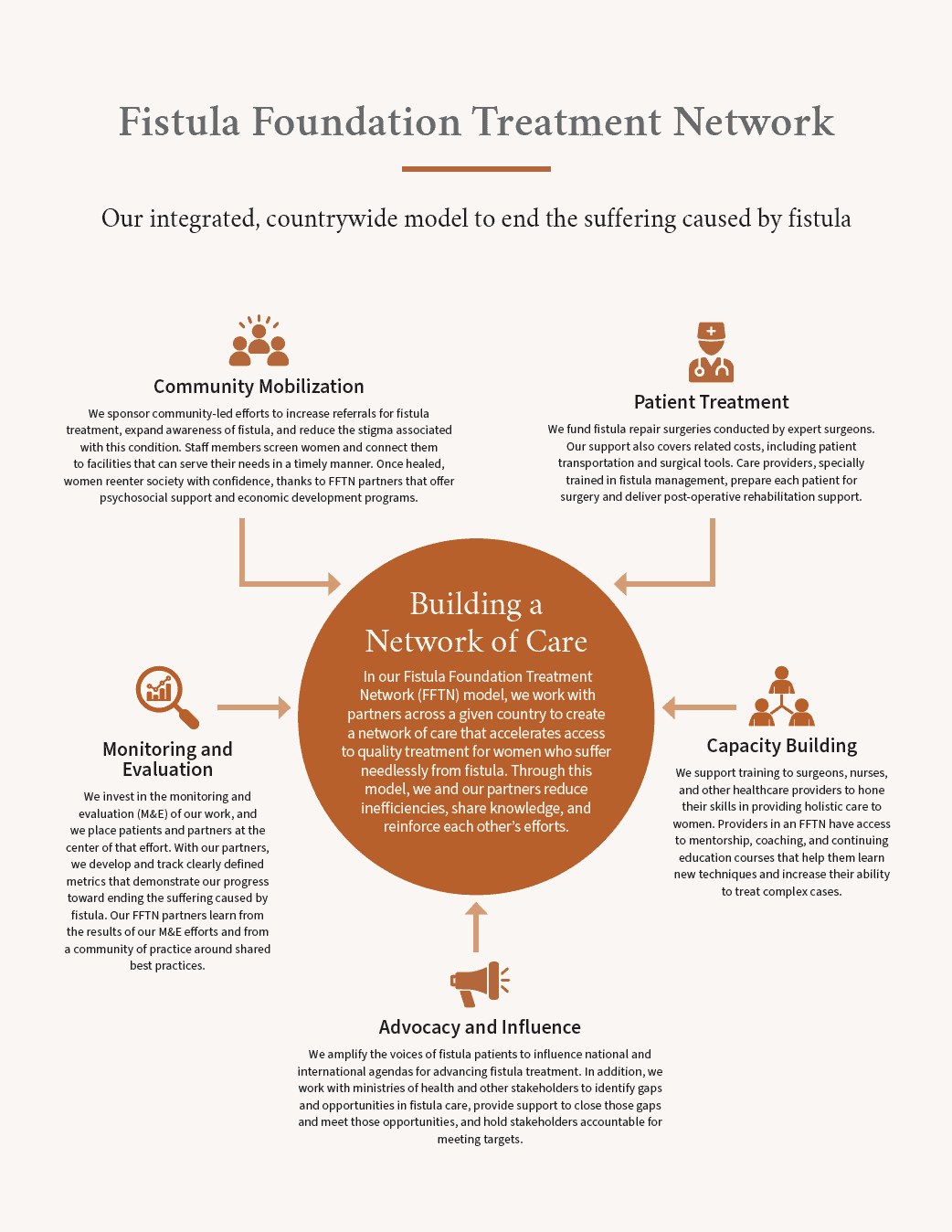
Second, we build long-term, in-country capacity by uniting surgeons, outreach partners, and government stakeholders to create sustainable access to care for tomorrow. In five of these countries—Kenya, Zambia, the Democratic Republic of Congo, Tanzania, and Nigeria—we’ve established a robust, countrywide model of care called the Fistula Foundation Treatment Network (FFTN).
Pam LowneyTwo bedrock truths guide everything we do: first, surgery is the only cure for fistula, and second, the faster we scale access, the sooner we restore women's health and futures. By expanding a proven model that is already transforming care in five countries across the African continent we can shorten wait times, shrink the backlog, and build a sustainable pipeline of qualified healthcare professionals that will end the suffering caused by fistula, once and for all.
Impact in Action
Since the launch of our first countrywide treatment network—in Kenya—in 2014, surgeries have soared and wait times for treatment have fallen. Still, our work is far from over, as each country faces high, unmet need for care. View the results from each countrywide treatment network to-date.
In Kenya, where we launched our first treatment network in 2014, the results are real. Wait times have fallen by 30%, and more than 18,000 life-changing surgeries have been provided since the network’s launch. Yet women treated today still report living with fistula for an average of six years before receiving care.
- Why Kenya? Despite significant development progress in recent decades, maternal health indicators in Kenya remain at disappointing levels. This is particularly true in the many rural parts of Kenya, where the majority of women deliver at home without a skilled birth attendant and far from any emergency obstetric care facilities. This has led to a high rate of obstetric fistula in rural Kenya.
- Impact to-date: Since its launch, our Fistula Foundation Treatment Network in Kenya has achieved tremendous results:
- 18,258 surgeries provided across 15 partners
- 15 surgeons and 103 nurses trained in fistula management
- 9,405 health service providers sensitized
- 1,766 community health volunteers trained
- More than 249,400 community outreach activities conducted
- More than 6.9 million community members reached through direct outreach activities, radio programs, and advertisements
Before the launch of the Fistula Foundation Treatment Network in Zambia, there were only four trained fistula surgeons in the entire country, severely constraining women’s access to timely, high-quality fistula care. With support from Johnson & Johnson, we launched the treatment network in 2017 to build Zambia’s long-term capacity for fistula care.
- Why Zambia? While economic indicators have improved over the past decade, unemployment remains a serious problem in Zambia. People in rural areas of the country face particular hardship, with the vast majority living in extreme poverty and lacking access to basic health care. Only half of the women in rural areas deliver with a skilled birth attendant—leading to high rates of maternal mortality and childbirth injuries such as obstetric fistula.
- Impact to-date: Since its launch, our Fistula Foundation Treatment Network in Zambia has achieved the following results:
- 3,063 surgeries provided across 8 partners
- Seven surgeons and 194 nurses trained in fistula management
- 3,016 community health volunteers and Safe Motherhood Action Group members trained to spread awareness of fistula and refer patients
- 2,538 rural healthcare providers trained on fistula identification and prevention efforts
- 5,469 local leaders sensitized on fistula
- 56,611 outreach visits carried out in 39 districts
- More than 1,054,339 people reached through radio programs and advertisements
In 2022, we launched the Fistula Foundation Treatment Network in the Democratic Republic of Congo (DRC) to build long-term capacity for fistula care in that country. In three short years, the FFTN delivered 11,194 surgeries to women in need across the DRC—a 245% increase in surgical volume. But an estimated 42,000 women are still suffering, and 6,000 new cases occur annually.
- Why Democratic Republic of Congo? Political upheaval and violent unrest have taken a heavy toll on DRC’s healthcare infrastructure. There is also a horrifying use of sexual violence in the country. For these reasons and others, DRC has been called “the worst place on earth to be a woman.”
- Over half of the Congolese population lives in rural areas, where health resources are spread thin—and in high demand. Even simply getting to the hospital can be close to impossible, with dirt roads that are completely flooded and impassable for months on end. All of these factors play a role in the DRC’s high incidence of obstetric fistula, and there is consistently more demand for fistula treatment than local hospitals can keep up with—contributing to a long backlog of Congolese women waiting for treatment.
- Impact to-date: Since its launch, our Fistula Foundation Treatment Network in the Democratic Republic of Congo has achieved the following results:
- 13,774 surgeries provided across 11 partners
- 62 surgeons and 481 nurses trained in fistula management
- 11,705 community members trained to spread awareness of fistula
- More than 137,263 people reached through radio programs and advertisements
- 130 outreach activities conducted
In 2023, alongside unveiling a five year strategic plan to build long-term capacity for fistula care, we launched the Fistula Foundation Treatment Network in Tanzania. The country faces one of the highest maternal mortality rates in sub-Saharan Africa, and for every woman who dies in childbirth, an estimated 20 other women suffer from a long-term disability such as obstetric fistula.
- Why Tanzania? Maternal health indicators have been improving in Tanzania, but there is still a long way to go. In cities, nearly all women deliver in hospitals—but more than 70% of the Tanzanian population lives in rural areas, where health care remains difficult to access.
- In Tanzania, women with fistula suffer for eight years on average before finding help. During that time, they experience significant emotional trauma—too often, fistula patients are shunned by their communities and abandoned by their husbands. Due to the isolating nature of fistula, many Tanzanian women do not know that their condition is treatable, and blame themselves for their misfortune or believe that they are cursed.
- Impact to-date: Since its launch, our Fistula Foundation Treatment Network in Tanzania has achieved the following results:
- 4,378 surgeries provided across seven partners
- 17 surgeons and 271 nurses trained in fistula management
- 1,601 community members trained to spread awareness of fistula
- More than nine million people reached through radio programs and advertisements
- 3,256 outreach activities conducted
Nigeria represents both the greatest need for care and the greatest opportunity for progress. Our FFTN in Nigeria—launched in 2025—leverages government partnerships and local expertise to deliver coordinated care at unprecedented scale. Our surgical volumes have more than tripled in three years—from 555 in 2022 to 2,034 in 2025. But the need for care is staggering.
- Why Nigeria? Nigeria faces Africa’s largest burden of obstetric fistula, and it’s no wonder, given a host of alarming maternal health indicators:
- Women have a 1 in 19 lifetime risk of maternal death
- Only half of all births are attended by skilled medical professionals
- Early marriage, adolescent pregnancy, and rural isolation drive high rates of obstructed labor that result in childbirth injuries, leaving tens of thousands of women suffering—many for years or even decades
- Our three-year growth plan: By 2028, the FFTN in Nigeria aims to:
- provide 8,400+ surgeries across 10 partners
- train dozens of providers
- restore nearly 53,577 years of healthy life
- generate $113.76 million in total lifetime productivity
- establish Nigeria as a model for sustainable, locally led fistula care at scale

